As more and more Ambulatory Surgery Centers (ASC) came across our bidding desk, the question emerged – is the Phoenix market becoming too saturated with ASCs? Overwhelmed by this speculative possibility, the nerd in me emerged, and I lost the next two days of my life researching the future ambulatory care in Arizona. I have read nearly every report possible from the Centers for Medicare & Medicaid Services rural strategies, the history of ASCs, market predictors for ASCs, and the Commercial Construction Index. Buckle in and grab a snack because this one is a wild ride.
After amassing nearly 67 pages of notes, I spent the last few days mulling over this information and figuring out how to put it in easily digestible bites for you!
So let’s start with this…
What the hell is an ASC, where did they come from, and why are they so immediately popular?
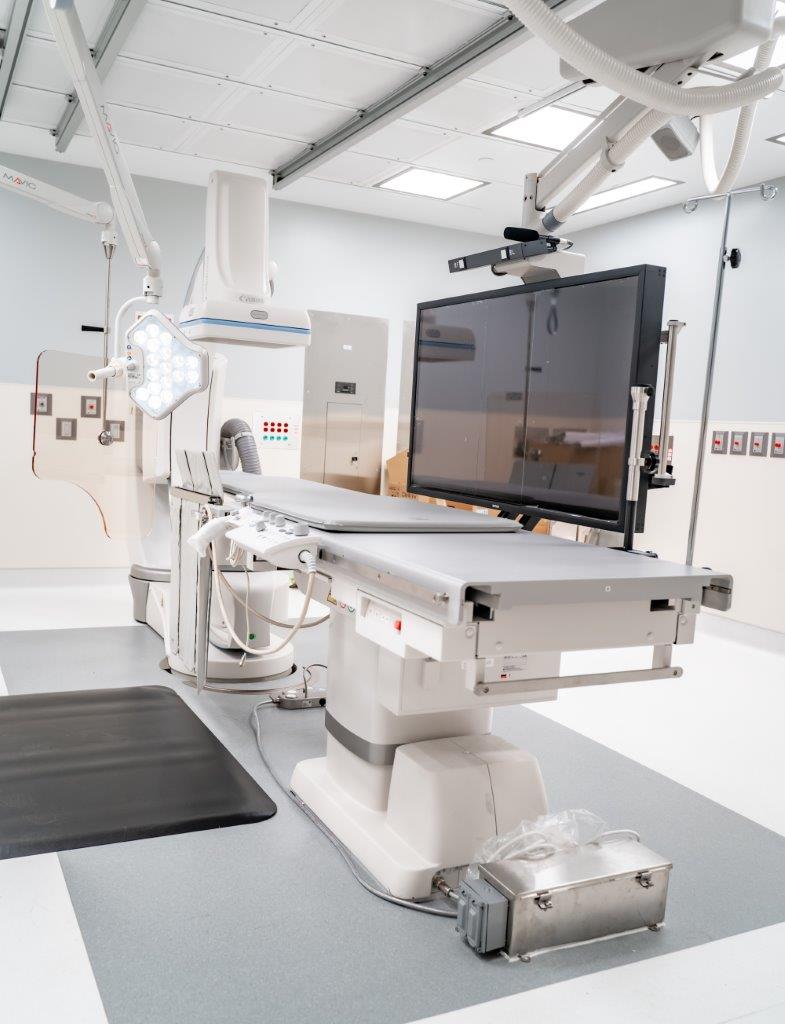
An ASC means an Acute Surgery Center. For ordinary people, this means you have a surgery done, not in a hospital or medical tower, and walk out (i.e., ambulatory). An ASC is clinically identical to an operating room in a hospital. The only difference is that the building you walk into isn’t a hospital. The only catch: you don’t require an overnight stay. Phoenix was the birthplace of ASCs in the 1970s when two doctors got fed up with hospitals outdated equipment, operating room delays, and the molasses of hospital decision-making.
Fast forward to today, and there are over 6,000 ASC’s in the USA, with over 90% of them having physician ownership. Keep in mind that big business has also found the opportunity. Groups like USPI (United Surgical Partnerships Institute) announced a $1.2B merger with SurgCenter and currently represent over 440 ASCs in 35 states. These are a group of people that figured out how to take the burden of operations (coding, billing, scheduling, human resources, etc.) off the doctor’s plate and offer ownership, albeit minority share.
So, come again – why is this exciting to doctors? If you have ever met a doctor, you might have noticed that they appreciate their autonomy. And suppose you have the pleasure of meeting a surgeon. In that case, you know they love efficiencies and cutting-edge equipment as much as I love spreadsheets. ASCs offer physicians and small groups a ton more money related to the procedure they perform. They can self-select equipment and upgrades, own the real estate, and when they get sick of cutting people open, they have the licensed real estate to sell!
Here are some ASC Quick facts for the nerds.
o 278 of the nation’s ASCs are multi-specialty (they do more than just your knee)
o The average ASCs has 4 ORs & 2 Procedure rooms (in Arizona, we most commonly see 2 ORs and a procedure room and about 10,000sq in space)
o ASCs average 5,000 cases per year (1,200 per OR and 1650 per procedure room)
o 53% commercial payors
o Less than 1% patient cancellation
o 50% faster surgical turnover
o An average of 31 people on staff. Sixteen RN’s, ten MDs, seven surgery technicians, and nine administrators. I would argue that we see the staff size much smaller in Arizona, with a lot of single to three surgeon groups.
o Cost to run an ASC = $15/min
o Cost to run an OR in a Hospital = $40/minute
o ASC see 50% greater volume per OR than a hospital
o The profit margin for ASC ownership is more significant than 40%

Sounds great on the operating side of the money train. But dirt and construction cost way too much in Arizona right now; how do they start in this market?
Yes, all the costs on the planet Earth are increasing. Despite the increase of (labor/supplies/materials/real estate), ASCs continue to be a hot purchase opportunity. The only bad news is that only 2% of ASCs sold annually. If you can find that unicorn, grab it. If not, it will cost you between $5 million and $10 million to build an average ASC with 2-4 operating rooms. If you want the Taj Mahal Hall, we can introduce you to great interior people.
The Center for Medicare & Medicaid Services: Who are they? And why should I care?
The CMS determines the ‘charge master.’ The chargemaster is the Wizard of Oz machine that tells Medicare and Medicaid how much they pay for the procedure or diagnosis. And even if you are not in these federal payor buckets, you need to pay attention to what procedures are funded. Eventually, whatever Medicare and Medicaid pay for, the commercial payors follow. Thus, your access to healthcare adapts.
The CMS pays hospitals way more money to do the same procedure than in an ASC licensed facility. Regardless of the reimbursement gap, ASC docs still make more money, and patients still pay less, and outcomes are all-around better. CMS is currently trying to pay ASCs more to continue the patient flow in this “outpatient” direction.
So let me get this straight, an ASC puts more money into the pockets of doctors, but what does that mean for the patients?
More good news is coming your way. Patient care is improved tremendously, systems and technology are newer and more advanced, and patients are in and out quicker. As a result of COVID-19, patient migration has drastically increased to booking surgeries in an ASC vs Hospital setting; healthy people don’t want exposure to sick people.
Let’s talk more about money. How much are we talking?
ASC’s ran some cash through, and that train is only beginning to leave the station. In 2020 ASC in the United States saw a revenue of $36B. This is predicted to be $93B by 2024.
Why don’t hospitals just do this on their own?
It just doesn’t work that way. A non-profit hospital strategy officer can’t go to the Board of Directors and say, “I have this great business case to start this new business model. All you have to do is purchase the real estate, move the surgeons out of the hospital (who are you key revenue drivers), hire additional support staff (during a massive nurse shortage), and take a few years to figure out ASC outpatient billing and coding. Now, can you approve $10 million so I can get started?”
I don’t think so. Career-ender.
Let’s look at it from a different lens. That same strategy officer can go to the board of directors and pitch, “I have a group of ASCs who, if we acquire, will come with the surgeons, staff, a billing treadmill, updated equipment, and federally licensed piece of real estate. Can you please approve $18 million (average sale price), and we will have an instant outpatient model that we can slap our brand on.”
You might recall when you saw the first urgent care take over your neighborhood blockbuster, and you thought, “What in the heck is an urgent care?” Welp, a group of businesspeople, saw this charge master pivot and sold their chain of 30 Arizona FastMeds to Honor Health in September of 2020.
Career-ender (the good kind)!
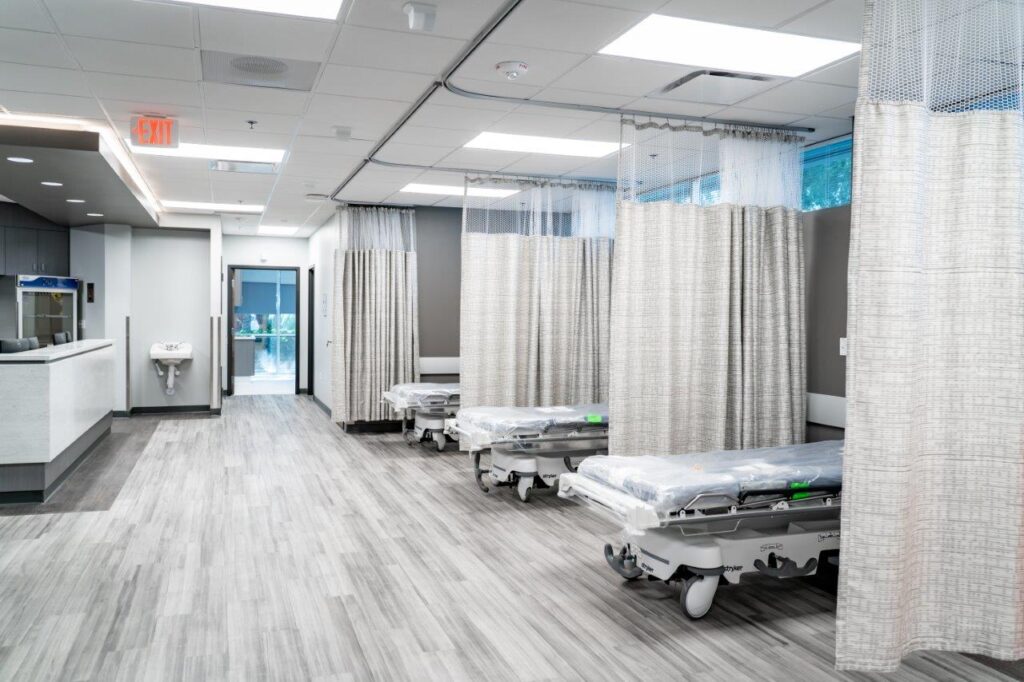
Phoenix Heart Ambulatory Surgery And Electrophysiology 
Phoenix Heart Ambulatory Surgery And Electrophysiology 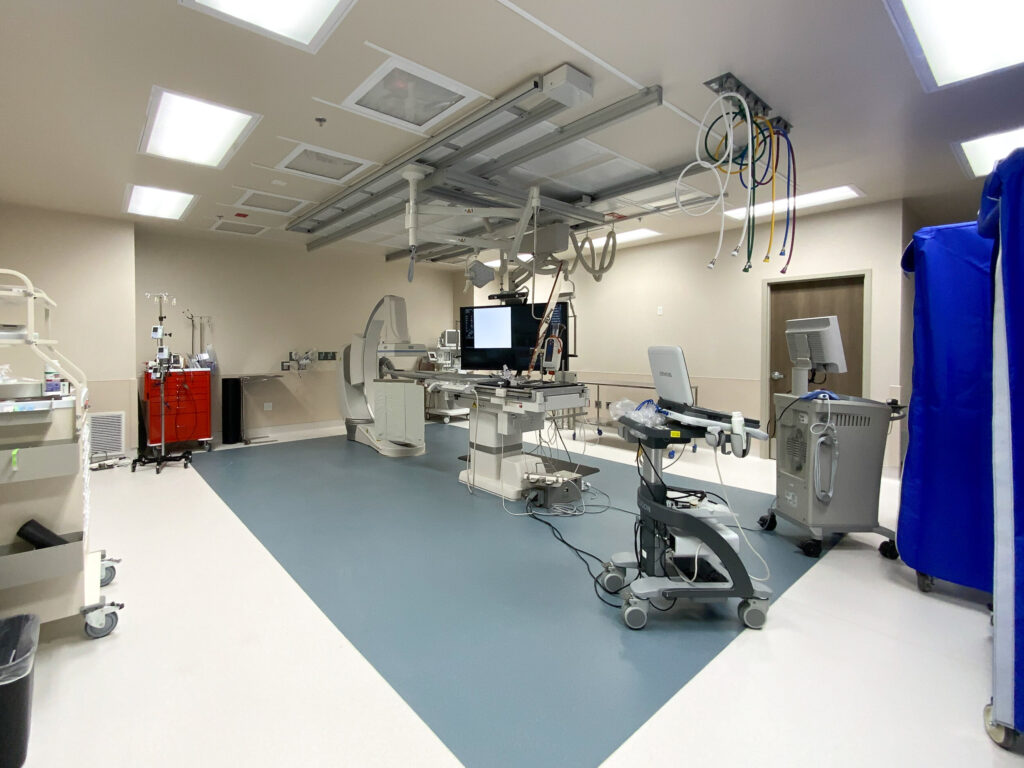
Apricus Surgery Center Avondale 
Regency Multispecialty ASC 
Regency Multispecialty ASC 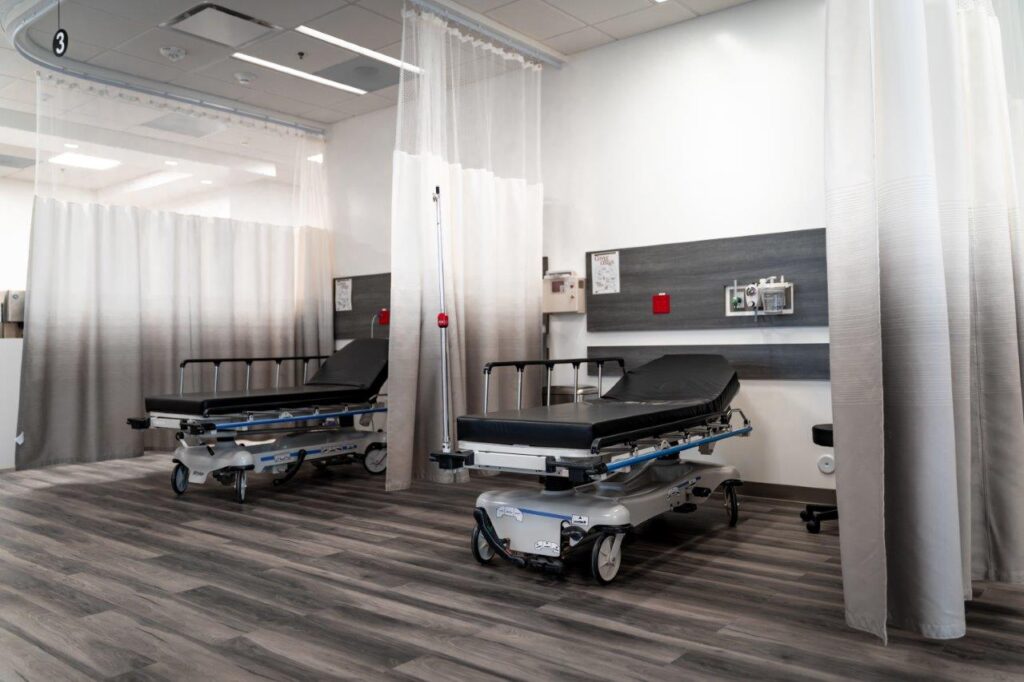
Regency Multispecialty ASC 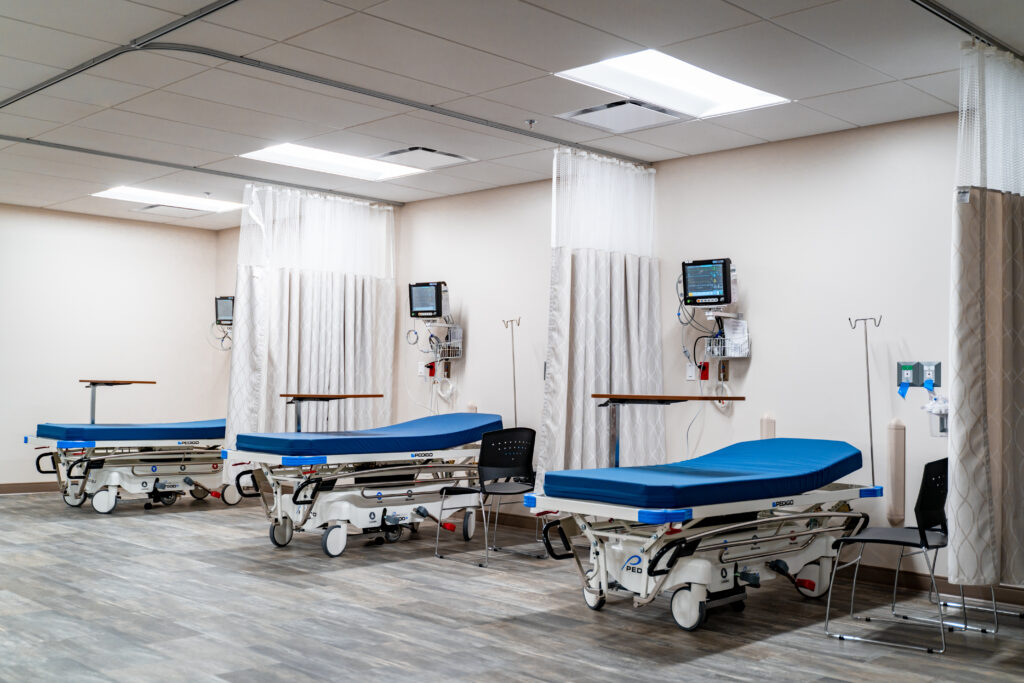
Apricus Surgery Center 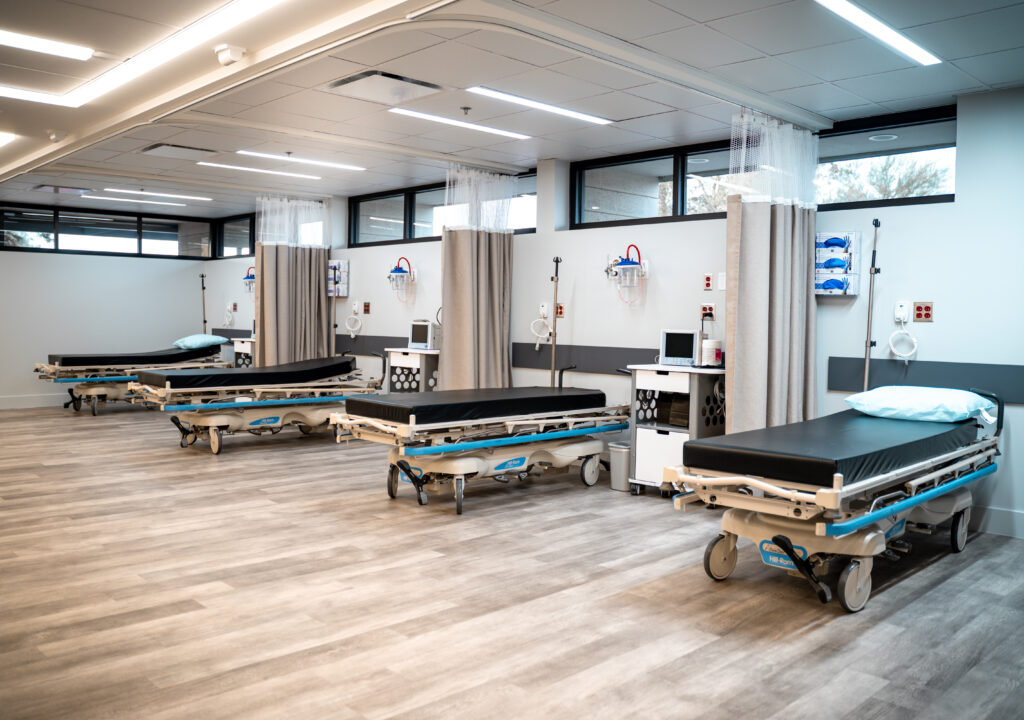
Civic Center Medical Plaza 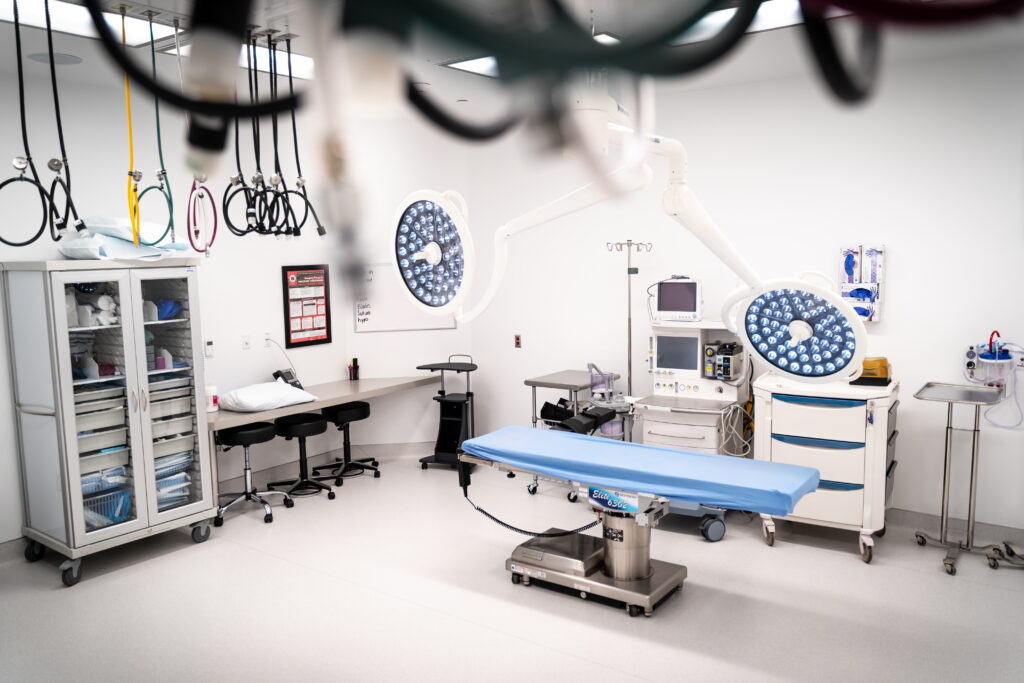
Civic Center Medical Plaza
A few more resources to show how the model is working and how hot the Arizona ASC market is comparative to the USA. Oh, and one of the fastest-growing populations as well.
https://www.honorhealth.com/healthy-living/honorhealth-fastmed-joint-venture
https://www.beckersasc.com/new-asc-development/all-255-new-ascs-by-state-in-2021.html